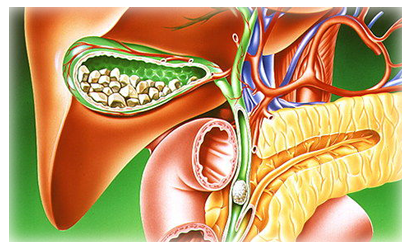 
Cotton, M.D., MUSC Gastroenterology and Hepatology professor and study author. “These findings do not support the use of ERCP and sphincterotomy for these patients,” said Peter B. Many patients have prolonged and expensive hospital stays, and some die, according to background information in the article. Procedure-related pancreatitis rates are 10 to 15 percent, and perforations may occur. The value of this endoscopic intervention is unproven and the risks are substantial. Of these patients, some undergo biliary or pancreatic sphincterotomy, (a surgical incision of a muscle that contracts to close an opening) or both. That dysfunction involves a muscle at the juncture of the bile and pancreatic ducts and the small intestine that controls the flow of digestive juices. Many of these patients undergo a procedure called endoscopic retrograde cholangiopancreatography or ERCP, which involves the use of an endoscope to inspect the pancreatic duct and common bile duct in the hope of finding small stones or other pathology or in an effort to address suspected sphincter of Oddi dysfunction. Most of these patients have no significant abnormalities on imaging or laboratory testing, and the cause of pain remains uncertain. More than 700,000 patients undergo gallbladder removal each year in the United States, and at least 10 percent report continued pain post-surgery. In certain patients with abdominal pain after gallbladder removal (cholecystectomy), undergoing an endoscopic procedure involving the bile and pancreatic ducts did not result in fewer days with disability due to pain, compared to a placebo treatment, according to a study in the May 28 issue of JAMA.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
